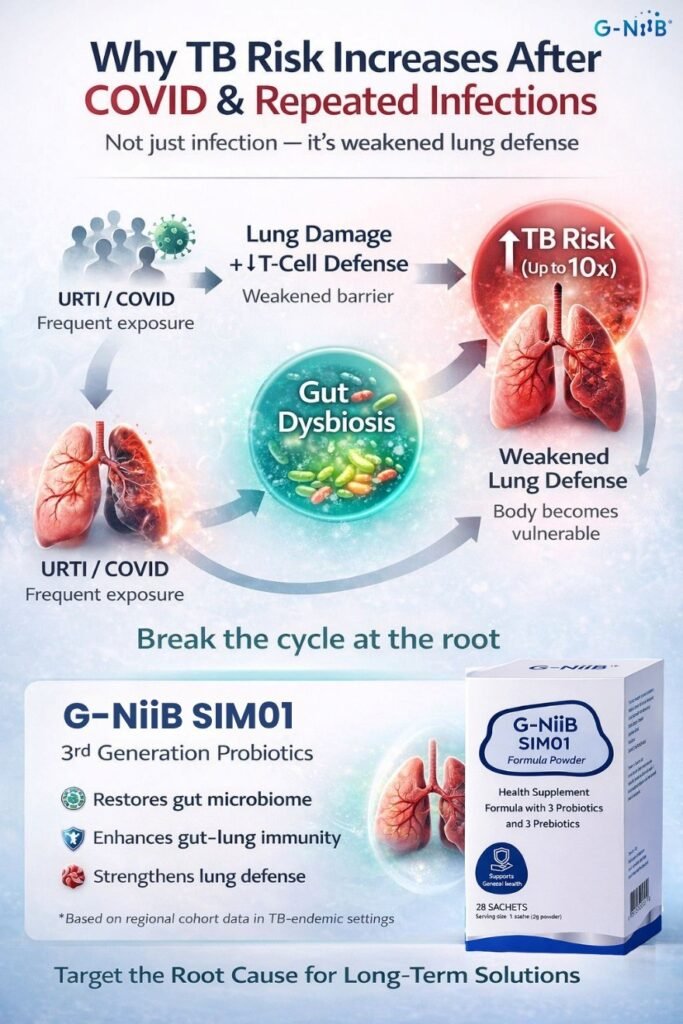
Why Strengthening Lung Defense Starts from the Gut
A Growing Respiratory Health Concern in Malaysia
Tuberculosis (TB) remains a significant public health challenge in Malaysia, with persistent incidence driven by urban density, comorbidities, and ongoing transmission. At the same time, upper respiratory tract infections (URTI), including common viral infections such as influenza, cold viruses, and COVID-19— are highly prevalent, especially in crowded environments.
While these conditions are often viewed separately, increasing evidence suggests they are biologically interconnected through weakened lung defense and immune dysregulation.
URTI and COVID-19: The First Hit to Lung Defense
URTI and viral respiratory infections are typically considered mild and self-limiting. However, repeated or severe infections, particularly COVID-19 pneumonia, can have deeper consequences:
- Damage to the respiratory lining (epithelium)
- Disruption of mucosal immunity
- Persistent inflammatory responses
- Alteration of the respiratory microbiome
This results in a state of impaired lung defense, where the body becomes more vulnerable to secondary or opportunistic infections.
Strong Clinical Signal: COVID-19 and TB Risk
Emerging regional data has highlighted how significant this risk can be.
In a Southeast Asian cohort:
- Patients with COVID-19 pneumonia had nearly a 10-fold higher hazard of detectable active pulmonary TB within the first 30 days
- The risk remained more than 7-fold higher beyond 30 days
This is a critical insight: Severe respiratory infections are not isolated events—they can significantly increase susceptibility to TB by weakening lung defense.
How URTI Increases the Risk of Tuberculosis
TB infection occurs when Mycobacterium tuberculosis enters the lungs. In healthy individuals, the immune system may contain it.
However, repeated URTI and viral infections do not just cause temporary illness, they initiate a damaging cycle that weakens lung defense and increases TB risk.
The Vicious Cycle of URTI → Lung Damage → TB
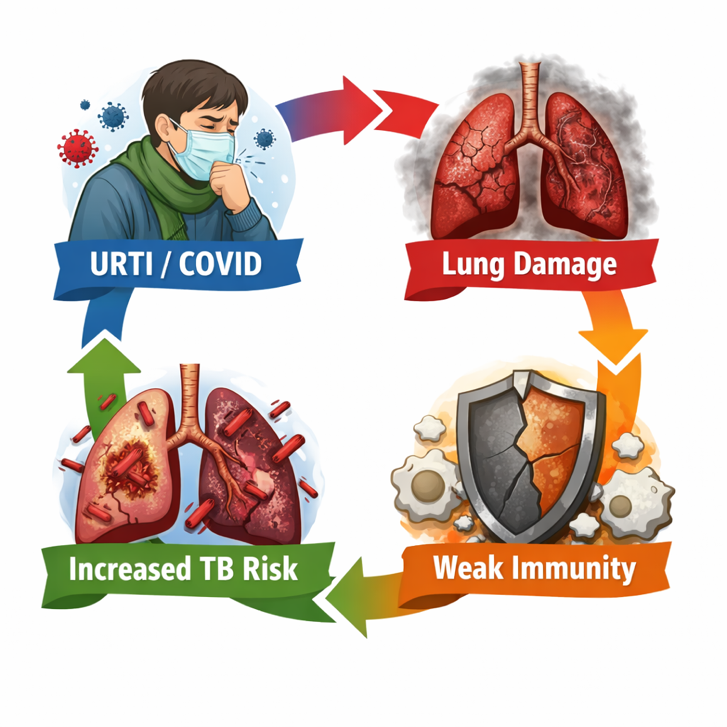
1. Barrier Breakdown
- Damage to airway lining allows easier entry and colonization of TB bacteria
2. Immune Dysregulation
- Overactive inflammation damages tissue
- Suppressed immune surveillance reduces bacterial control
3. Compounding Exposure Risk
In Malaysia’s crowded settings:
- Higher exposure to airborne infections
- Increased transmission of both URTI pathogens and TB
Why These Diseases Co-Exist in Malaysia
The overlap is not coincidental. Shared drivers include:
- High population density and crowd exposure
- Frequent respiratory infections
- Chronic conditions (e.g., diabetes, smoking)
- Environmental and lifestyle factors

Together, they form a continuum:
URTI, COVID-19, and TB are interconnected stages of respiratory vulnerability—not isolated diseases.
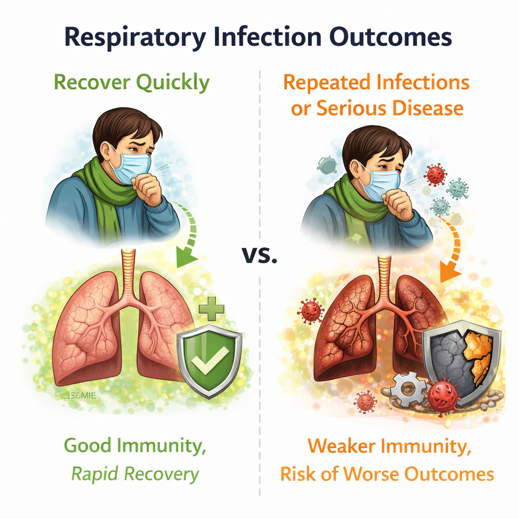
Why:
- Some individuals recover quickly?
- Others experience repeated infections or progression to more serious disease?
The Missing Link: The Gut–Lung Axis
Modern science has uncovered a critical connection – the gut–lung axis:
- The gut microbiome regulates systemic immunity
- Immune signaling from the gut influences lung defense
- Dysbiosis (microbial imbalance) weakens immune resilience
Importantly:
Respiratory infections can disrupt gut microbiota, and gut dysbiosis can further impair lung immunity— a two-way relationship.
Why Conventional Approaches Are Not Enough
Current strategies focus on:
- Treating infection (antibiotics, antivirals)
- Managing symptoms
However, they often do not address the root cause:
- Microbiome imbalance
- Immune dysregulation
- Long-term susceptibility
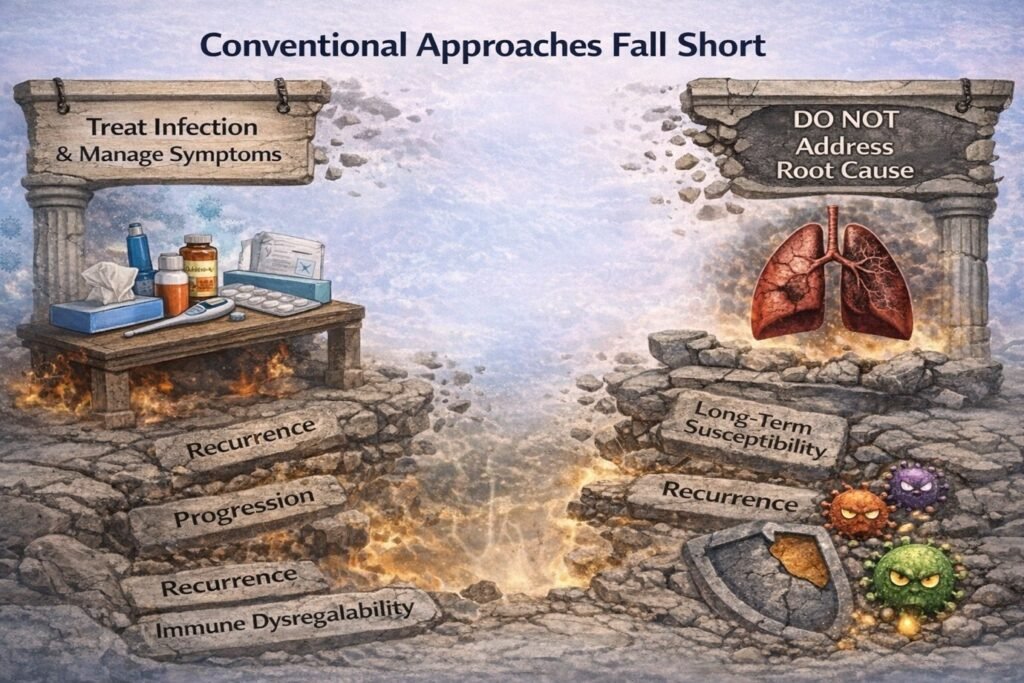
As a result, recurrence and progression remain common.
A New Approach: Targeting the Root Cause
3rd Generation Probiotics – A Potential Game Changer

Unlike conventional probiotics, 3rd generation probiotics (e.g., SIM01) are developed based on The Chinese University of Hong Kong’s unique metagenomic and AI discovery engine, are designed using:
- Disease-specific microbiome insights
- Precision strain selection (metagenomics & AI-driven)
- Targeted restoration of beneficial bacteria
How SIM01 Fits into This Model
- Helps restore specific gut microbiome balance
- Supports immune modulation (not suppression)
- Reinforces the gut–lung axis
- Enhances resilience against repeated respiratory infections
In the context of URTI, COVID-19, and TB:
Instead of only reacting to infection, SIM01 targets the underlying immune foundation.
Putting It All Together
In Malaysia today:
- URTI is common and often underestimated
- COVID-19 has added a new layer of immune disruption
- TB remains endemic
Key Insight
Repeated or severe respiratory infections— including COVID-19— can weaken lung defense and significantly increase vulnerability to TB, with studies showing up to a 10-fold increase in risk in the early phase.
Conclusion: From Infection Control to Immune Resilience
Exposure to infections may be inevitable— especially in crowded environments. The focus must therefore shift from:
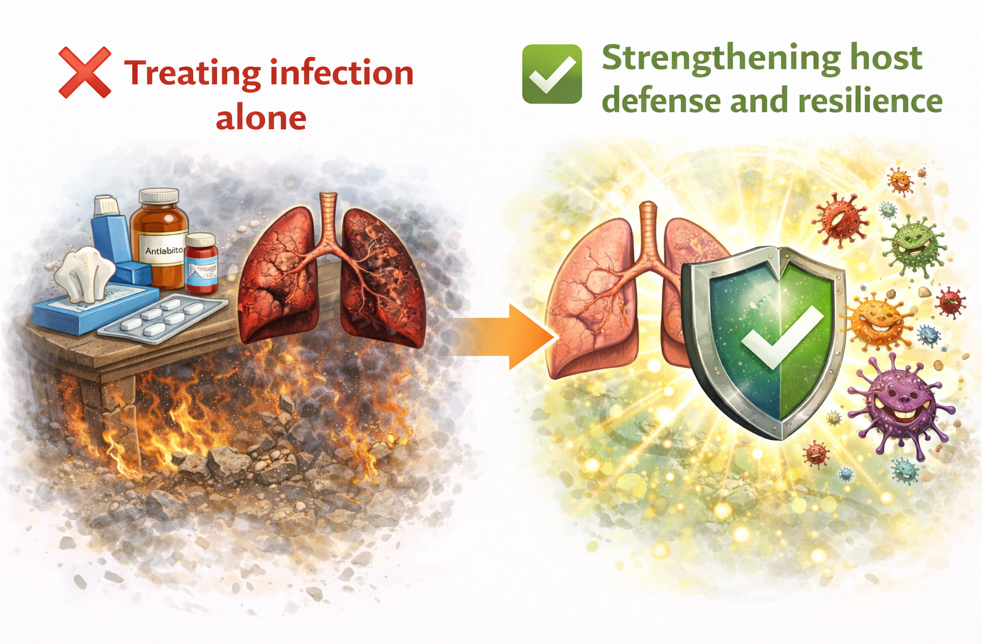
This is where innovations like 3rd generation probiotics (SIM01) offer a new direction:
Target the Root Cause

Restore Microbiome

Strengthen Immunity

Reduce Long-Term Risk